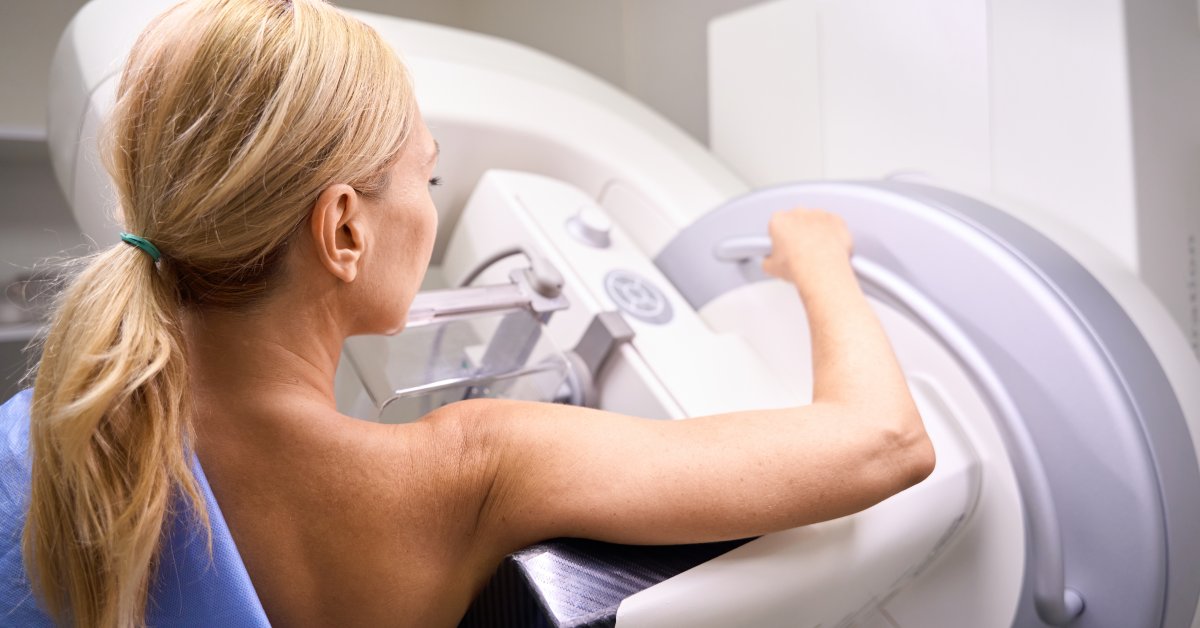
Most women should start mammogram screenings for breast cancer at age 40, and get screened every other year until they reach age 75, according to new recommendations from an expert panel.
The U.S. Preventive Services Task Force (USPSTF), which is an independent group of experts funded by the government, regularly reviews data and makes recommendations on health issues, and many health providers follow them. It decided to revise its advice on mammogram screening that was last issued in 2016. That guideline said women should start regular mammogram screening every other year beginning at age 50, and that women ages 40 to 49 should discuss with their doctors the best screening regimen for them.
Here’s what to know about the latest change.
When should most women get their first mammogram?
The new recommendation is based on additional evidence that has emerged since 2016, says Dr. John Wong, vice chair of USPSTF. According to data from the National Cancer Institute, death rates from breast cancer for women in their 40s began increasing by 2% annually in 2015, and that trend justified a change in the recommendations to start screening a decade earlier. “Our current data shows that this recommendation could potentially save as many as one out of five women who would otherwise die if they waited to be screened until they were 50,” says Wong. “That’s potentially saving 25,000 women from dying of breast cancer. We think that’s a big win.”
Read More: Why Are So Many Young People Getting Cancer?
It’s not clear what is contributing to increased risk among women in their 40s. But Wong says the task force analyzed whether USPSTF’s recommendation around that time—to start mammograms once women turned 50 rather than 40, as the group’s previous guideline advised—was a factor, as some advocates had warned. “Screening rates remained consistent throughout that period,” he says. “So that’s not the cause.” The most recent data do include different populations of women, however, incorporates different types of screening and treatment options that weren’t available when the previous populations were studied, so more screening may be leading to more diagnoses, for example.
The current recommendation now brings the USPSTF’s guidance more in line with that of other health groups including the American Cancer Society. That group advises women to start screening at age 45 annually until age 54, then every other year.
Why did the recommendation change?
Wong says the new guidelines reflect the changing benefits and risks of screening and its consequences, which include additional testing, as well as the risk of false positives. The increased risk of dying from breast cancer among women in their 40s tipped the balance in favor of beginning screening earlier.
What about women with dense breasts?
About half of women in the U.S. have dense breast tissue; for them, mammograms are less reliable at detecting cancer. The task force is less clear about whether these women should follow the same recommendations. It says the evidence supporting the benefits of additional screening—with MRIs or ultrasounds, which doctors often recommend if mammograms are negative or inconclusive—isn’t “sufficient.” Wong says more research is needed to understand if those additional imaging tests help women to get diagnosed earlier and ultimately allow them to live longer. “We just don’t have clear evidence at this time,” he says.
Will insurance cover mammograms starting at age 40?
All insurance companies (with few exceptions) must cover the cost of mammograms with no co-pay for women who get them as part of regular screening beginning at age 40. That’s part of the Protecting Access to Lifesaving Screenings Act that was passed by Congress in 2019. Because of this act, the new guidelines should not affect insurance coverage of mammograms for women in their 40s.
Read More: A 5-Minute Quiz Revealed Olivia Munn’s Breast Cancer Risk. You Can Take It Too
But since the task force says the evidence for additional screenings is “insufficient,” women with dense breast tissue may still have to pay out of pocket for additional tests beyond a mammogram. That could lead to lower follow-up for these women and ultimately may delay any breast cancer diagnoses until later stages, when the disease is harder to treat. “We worry about what it means for access and utilization for those women, to say that there is inconclusive evidence to support supplemental imaging,” says Molly Guthrie, vice president of policy and advocacy at the Susan G. Komen Breast Cancer Foundation.
Guthrie notes that already, many states require that mammography centers notify women if they have dense breast tissue, so they and their doctors are aware that the mammogram readings may have missed potential red flags for cancer. That requirement will apply to all mammography facilities beginning this September, after the U.S. Food and Drug Administration, which regulates the facilities, issued a new rule last year mandating the information. “The FDA is trying to get to the point of pushing the conversation about dense breast tissue so women have a dialogue with their providers,” says Guthrie. “But if you are not doing anything to change coverage, you are not going to increase utilization.”
Wong stands by the task force’s conclusion, seeing it as an invitation for further study. “We would love to have sufficient evidence that would help women with dense breast tissue to live longer, healthier lives, and we are urgently calling for more research to obtain that evidence,” he says. “We always look at the latest and best science—and at the benefits and harms—to make recommendations that help people in this nation stay healthy and live longer.”